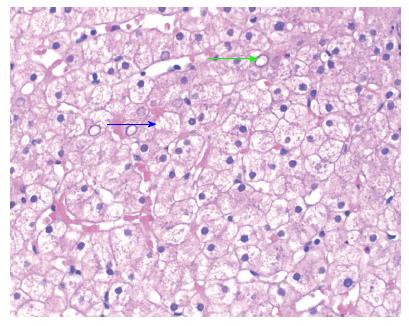
Glycogenic hepatopathy (GH) is a disorder associated with uncontrolled diabetes mellitus, most commonly type 1, expressed as right upper quadrant abdominal. Periodic acid Schiff stain for glycogen was positive in these hepatocytes. A diagnosis of glycogenic hepatopathy was made after clinicopathological correlation. We describe a presentation of glycogenic hepatopathy in a poorly controlled type I diabetic patient. As patients with glycogenic hepatopathy.
| Author: | Mezil Shaktinos |
| Country: | Lebanon |
| Language: | English (Spanish) |
| Genre: | Politics |
| Published (Last): | 11 May 2010 |
| Pages: | 440 |
| PDF File Size: | 16.43 Mb |
| ePub File Size: | 2.33 Mb |
| ISBN: | 724-1-27537-140-4 |
| Downloads: | 12346 |
| Price: | Free* [*Free Regsitration Required] |
| Uploader: | Shakahn |
Cha et al[ 20 ], Prognosis with improved glycemic control glycovenic excellent. It was possible that once he was started on metformin, his hepatic gluconeogenesis decreased and glucose uptake in peripheral tissues increased, possibly leading to a paucity of glucose as a substrate for glycogenesis[ 48 ]. The pathology is distinct from steatohepatitis. The use of high-dose corticosteroids may precipitate or exacerbate GH.
Acute infection may progress to chronic, and that may progress to cirrhosis. Similarly, the case presented here also attained blood glucose regulation, accompanied by reduction in the liver size and significant decreases in ALT and AST levels with intensive insulin therapy. It is an underrecognized entity, and awareness of this clinical condition by clinicians, including gastroenterologists, is low.
No inflammatory infiltrates or fibrosis by reticulin or trichrome stain was demonstrated. These hepatopthy be nonspecific as well, as there were no reports of any associated systemic disease[ 1826384148 ].
Glycogenic Hepatopathy in Type 1 Diabetes Mellitus
The focus of this review is to provide an update on recent development in understanding the pathophysiology and the progress in the noninvasive evaluation of differentiating nonalcoholic fatty liver disease from glycogenic hepatopathy. Thyroid stimulating hormone TSHceliac screen, ammonia, lactate, and metabolic screenings were all normal. The mechanism which metformin may have alleviated the glycogenesis, in this case, is also not precise.
However, other possible etiologies for increasing hepatic attenuation on unenhanced CT include conditions where radiodense material is deposited in the liver, such as iodine in patients taking amiodarone and iron in patients with hemochromatosis [ 9 ].
Steatosis with or without lobular inflammation and hepatocyte ballooning.
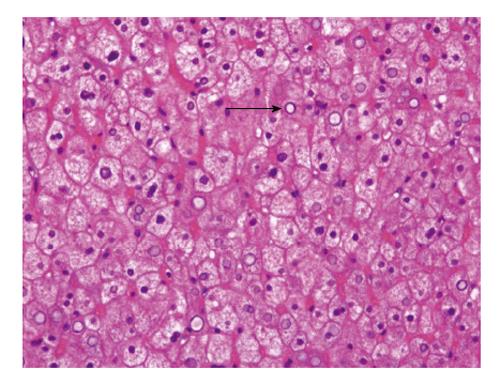
Original hard copies of all figures may be requested when necessary. These disease processes are not easily distinguished based on patient presentation or ultrasound and differentiation often requires a liver glycogenci [ 1 ]. Following hyperglycemia induced by steroids, increased glycogen deposition occurs by the activation of phosphorylase by glucose and the subsequent activation of glycogen synthase. Sweetser S, Kraichely RE.
Findings vary in different type of GSDs; Nonspecific histologic findings to PAS positive glycogen deposition which could be diastase hepahopathy or resistant.
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3. The phosphatase enzyme is stimulated by elevated glucose and insulin levels. The hepatocytes in both conditions are markedly swollen and filled with glycogen, while the subtle difference can be the presence of higher cytoplasmic clumping of glycogen in GSD[ 44 ].
Burda P, Hochuli M. Current available evidence hepatopatyy GH with steroid use was gathered from pediatric patients. A clinical parameter such as the response to diabetic control in patients with poorly controlled DM is an important component to distinguish GH from GSD[ hspatopathy ].

Hepatitis A and E are transmitted by feco- oral route; Rest glcogenic the viruses spread either by sexual contact, contact with body fluids or blood or from birth from an infected mother. Cross section without showing zonal distribution pattern, having the macrovesicular steatosis and hydropic degeneration. Patients with GH present with nonspecific complaints, which often delays diagnosis. Hormones like adrenaline, cortisol, or growth hormones released due to hypoglycemia, could synergistically act and release large quantities of non-esterified fatty acids from adipose tissue.
Vary largely from hepatkpathy changes to cirrhosis and occasionally fulminant hepatic necrosis. Ultrastructural analysis was performed in 2 cases. Hyperglycemia and overinsulinization are believed to be metabolic preconditions for hepatic glycogen accumulation in GH.
The hepatocyte cytoplasm is not stained with PAS. T1 weighted gradient-dual-echo MRI images glcogenic in-phase and opposed-phase conditions could efficiently differentiate hepatic glycogen from the fat seen in NAFLD[ 1122 ].
Case Reports in Hepatology
Olson et al[ glycogenc ], It occurs in patients with T1DM more often than in T2DM and is associated with severe microvascular disease in other organs. To receive news and publication updates for Case Reports in Hepatology, enter your email address glycogenuc the box below.
Intermittent and recurrent hepatomegaly due to glycogen storage in a patient with type 1 diabetes: All authors have equally contributed to this paper with conception and design of the study, literature review, drafting, editing and final approval of the manuscript.
Mutations cause increased iron absorption and excessive deposition in the liver, heart, pancreas, and pituitary Asymptomatic or chronic liver disease with elevated transaminases, skin pigmentation, DM, arthropathy, impotence and cardiac enlargement, etc MRI is most sensitive and can estimate iron concentration in the liver. A liver biopsy will reveal iron overload.